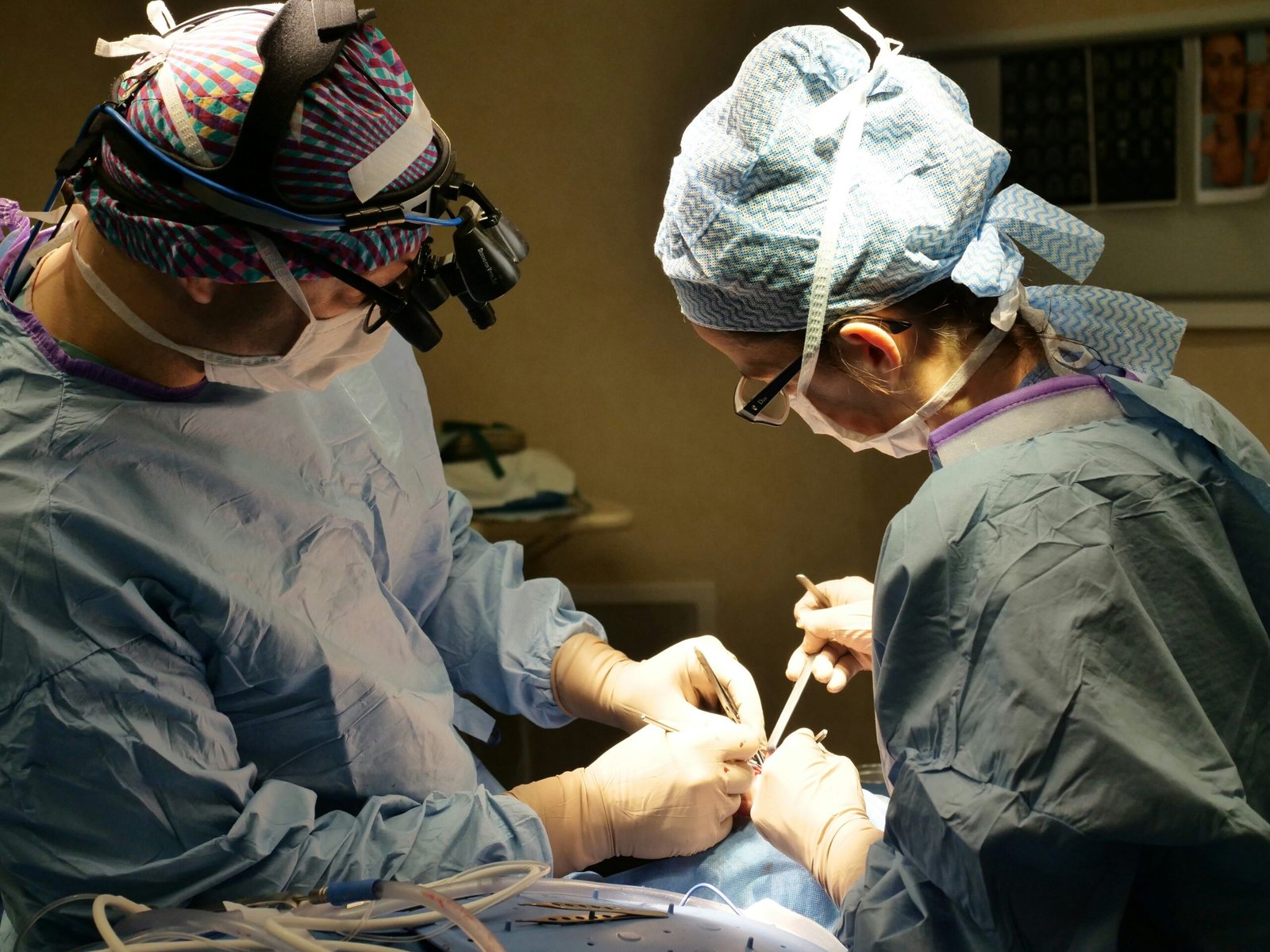
My career, as an orthopedic surgeon specializing in knee replacement, offers me a unique vantage point into the evolving landscape of musculoskeletal health. I dedicate my professional life to restoring function and alleviating pain for individuals grappling with debilitating knee conditions. This article, written from my perspective, will illuminate the multifaceted role of an orthopedic surgeon in the context of knee replacement, drawing upon current trends and challenges within the field.
When a patient walks into my office with chronic knee pain, it’s often after a long journey of conservative treatments – physical therapy, medications, injections. They’ve reached a point where their quality of life is severely compromised. This is where I, as their surgeon, enter the narrative.
Degenerative Conditions Leading to Surgery
The primary culprit in most knee replacement cases is osteoarthritis, a wear-and-tear disease that erodes the smooth cartilage cushioning the knee joint. Imagine the knee as a finely tuned machine, and the cartilage as the oil that keeps its moving parts gliding effortlessly. Over time, that oil can deplete, causing friction and damage. Other conditions, such as rheumatoid arthritis or post-traumatic arthritis, can also necessitate surgical intervention. I carefully evaluate the extent of this damage through physical examination, X-rays, and sometimes MRI scans, to determine if surgery is the most appropriate path forward.
Impact on Patient Quality of Life
The decision to undergo knee replacement is a significant one. I’ve seen firsthand how chronic knee pain can be a cruel thief, stealing independence, hobbies, and even the simple joy of a walk in the park. My role extends beyond the technical aspects of surgery; it encompasses understanding the profound impact this condition has on a patient’s life and guiding them towards a solution that promises a return to normalcy.
If you are considering knee replacement surgery, it is essential to understand the procedure and its benefits thoroughly. A related article that provides valuable insights into this topic is available at Orthopedic King. This resource covers various aspects of knee replacement, including indications for surgery, the surgical process, recovery expectations, and potential risks, helping patients make informed decisions about their orthopedic health.
The Role of the Orthopedic Surgeon in Pre-Operative Care
My commitment to a patient’s successful outcome begins long before they enter the operating room. Pre-operative care is a critical foundation.
Comprehensive Patient Evaluation
Before any decision is made, I conduct a thorough physical examination, review the patient’s medical history, and analyze diagnostic imaging. This comprehensive evaluation allows me to understand not only the severity of their knee condition but also their overall health status. Are there co-existing medical conditions that need to be managed? What are their expectations and goals for surgery? These are all questions I meticulously address.
Patient Education and Shared Decision-Making
One of my most important responsibilities is to educate patients about the procedure itself. I explain the different types of knee replacements – total knee arthroplasty (TKA) and partial knee arthroplasty – and the rationale for recommending a specific approach. I describe the surgical risks, potential benefits, and the expected recovery timeline. This process is about shared decision-making; I aim to empower patients to be active participants in their treatment plan, not just passive recipients. I often use anatomical models to illustrate the procedure, helping them visualize the journey their knee will undergo.
Optimizing Patient Health for Surgery
My team and I also focus on optimizing the patient’s health before surgery. This might involve referring them to other specialists for pre-operative clearance, managing chronic conditions like diabetes or high blood pressure, and encouraging lifestyle modifications such as smoking cessation or weight loss. A healthier patient is better equipped to undergo surgery and experience a smoother recovery.
Innovations in Knee Replacement Surgery
The field of orthopedic surgery is a dynamic one, constantly evolving with technological advancements. I make it my mission to stay at the forefront of these innovations to offer my patients the best possible outcomes.
Robotic-Assisted Arthroplasty
The advent of robotic-assisted arthroplasty has been a significant leap forward. From my perspective, this technology acts as a meticulous co-pilot, enhancing my precision during surgery. While my hands remain the primary drivers, the robotic system provides real-time data, allowing me to execute bone cuts and implant placement with unparalleled accuracy. Recent data, which I’ve observed firsthand, shows higher patient satisfaction and improved quality of life for those undergoing robotic-assisted total knee replacement. Crucially, the infection rates remain comparable to conventional surgery, dispelling some initial concerns about new technologies.
AI and Robotics for Precision and Alignment
Beyond robotic assistance in the operating room, artificial intelligence (AI) is transforming how I approach surgical planning. AI algorithms can analyze complex anatomical data, predict optimal alignment, and even suggest component placement with a level of sophistication that surpasses traditional methods. This prompts me and my colleagues to rethink some long-held surgical approaches. The synergy between AI-driven planning and robotic-assisted execution is like having a digital blueprint guiding a highly skilled craftsman, minimizing variability and maximizing precision.
The Shift Towards Outpatient Settings
One of the most remarkable shifts I’ve witnessed in my practice is the accelerating migration of orthopedic procedures, including knee replacements, to outpatient settings. This evolution is a testament to advancements in surgical techniques and anesthesia.
Minimally Invasive Techniques and Anesthesia
My focus, and that of my colleagues, on minimally invasive techniques has been instrumental in this shift. Smaller incisions, less tissue disruption, and improved pain management protocols allow for quicker recovery times. Concurrently, advances in anesthesia, particularly regional anesthesia like nerve blocks, significantly reduce post-operative pain and nausea, making it feasible for patients to recover comfortably at home rather than in a hospital bed. This transition to ambulatory surgery centers (ASCs) is not merely a logistical change; it represents a paradigm shift in how we deliver care, emphasizing patient comfort and efficiency.
Benefits and Challenges of Outpatient Surgery
The benefits of outpatient knee replacement are substantial. Patients often experience a reduced risk of hospital-acquired infections, a more comfortable recuperation in their own environment, and often, a lower overall cost. The convenience factor for both patients and their families is also a significant draw. However, this shift is not without its challenges. I must carefully select appropriate candidates for outpatient surgery, ensuring they have adequate home support and are medically stable. Moreover, the projected growth of about 6% annually through 2030 in outpatient orthopedic volume requires robust infrastructure and coordinated care to maintain high standards of patient safety and outcomes.
If you are considering knee replacement surgery, it is essential to understand the various aspects of the procedure and its benefits. An informative resource that can help guide you through this journey is an article on orthopedic surgeons specializing in knee replacements. You can read more about it by visiting this link, which provides valuable insights into the qualifications and expertise of knee doctors in Thane. This information can be crucial in making an informed decision about your treatment options.
Post-Operative Care and Long-Term Outcomes
| Metric | Details |
|---|---|
| Average Surgery Duration | 1.5 to 2 hours |
| Success Rate | 90% – 95% |
| Average Hospital Stay | 2 to 4 days |
| Recovery Time | 3 to 6 months |
| Common Complications | Infection, Blood Clots, Implant Loosening |
| Experience Required | 5+ years in orthopedic surgery, specialized in knee replacement |
| Patient Satisfaction Rate | 85% – 90% |
| Follow-up Frequency | 1 week, 6 weeks, 3 months, 6 months, 1 year post-surgery |
My commitment to a patient doesn’t end when the surgical dressings are applied. The post-operative phase is equally, if not more, critical for a successful recovery.
Comprehensive Pain Management Strategies
Post-operative pain management is paramount. I utilize a multimodal approach, combining regional anesthesia, oral pain medications, and sometimes nerve blocks, to keep patients as comfortable as possible. This proactive approach to pain allows them to engage more effectively in physical therapy, which is the cornerstone of rehabilitation.
Physical Therapy and Rehabilitation
I always emphasize to my patients that surgery is only half the battle; physical therapy is the other, equally important half. Rehabilitation begins almost immediately after surgery, focusing on restoring range of motion, strengthening the surrounding muscles, and improving balance. I work closely with physical therapists to tailor individualized recovery plans, addressing real-world challenges such as swelling and implant durability, to ensure optimal long-term mobility and improved quality of life. The patient’s dedication to their therapy regime is like tending to a newly planted sapling; consistent care ensures robust growth.
Monitoring Implant Durability and Longevity
The longevity of the knee implant is a crucial aspect of my post-operative care. I regularly monitor patients through follow-up appointments and imaging to assess implant position, wear, and overall function. My goal is to ensure the implant provides years, if not decades, of pain-free mobility. Research consistently focuses on implant design and materials science to enhance durability, and I integrate these advancements into my practice.
Navigating the Healthcare Landscape: My Perspective
Beyond the clinical aspects of my work, I find myself increasingly navigating the complex and often challenging terrain of the healthcare system.
Declining Reimbursement and Administrative Burdens
One of the most pressing concerns for me and my practice is the declining reimbursement for procedures like total knee arthroplasty. Coupled with increased payer scrutiny, this creates a situation where the financial viability of providing high-quality care is under constant pressure. We are forced to be more efficient, to automate processes, and to restructure operations to weather these economic headwinds. Prior authorization requirements, a seemingly endless bureaucratic hurdle, add significant administrative burdens, diverting valuable resources and staff time away from direct patient care. It’s like trying to navigate a ship through a storm with dwindling supplies.
Importance of Accurate Coding and Billing
In this environment of declining reimbursements, accurate CMS coding and billing become absolutely essential. The risk of underbilling for complex procedures is high, and any inaccuracies can have significant financial repercussions for my practice. I, therefore, rely heavily on a highly competent administrative team to ensure meticulous documentation and precise billing practices. This administrative rigor, though not directly related to the surgical act itself, is vital for maintaining the operational health of my practice and, by extension, my ability to continue providing specialized care to my patients.
My journey as an orthopedic surgeon specializing in knee replacement is one of continuous learning, adaptation, and dedication to improving the lives of my patients. I am not just a technician of bone and cartilage; I am a guide, an educator, and a partner in their pursuit of renewed mobility and a life free from debilitating pain. The advancements in my field, from robotics to outpatient care, are exciting, and I embrace them with the conviction that they will continue to enhance the quality of care I can offer.
FAQs
What qualifications should an orthopedic surgeon for knee replacement have?
An orthopedic surgeon specializing in knee replacement should have completed medical school, followed by a residency in orthopedic surgery. Additional fellowship training in joint replacement or specifically knee surgery is highly recommended. Board certification in orthopedic surgery is also an important credential indicating expertise.
When is knee replacement surgery recommended?
Knee replacement surgery is typically recommended for patients with severe knee pain and disability caused by conditions such as osteoarthritis, rheumatoid arthritis, or traumatic injury, especially when conservative treatments like medication, physical therapy, and injections have failed to provide relief.
What types of knee replacement procedures are available?
There are mainly two types of knee replacement procedures: total knee replacement, where the entire knee joint is replaced, and partial knee replacement, where only the damaged part of the knee is replaced. The choice depends on the extent of joint damage and the surgeon’s assessment.
What should I expect during recovery after knee replacement surgery?
Recovery typically involves pain management, physical therapy, and gradual return to normal activities. Most patients can walk with assistance within a day or two after surgery and continue rehabilitation for several weeks to months to regain strength and mobility.
How can I find a qualified orthopedic surgeon for knee replacement?
You can find a qualified orthopedic surgeon by seeking referrals from your primary care physician, checking credentials and board certification, reading patient reviews, and consulting with surgeons who specialize in knee replacement surgery at reputable medical centers.